|
|
In August, 2023 Erin Braasch, Executive Director of WNC Health Network, interviewed Norma Duran Brown, Executive Director of UNETE. Norma shared about UNETE’s partnership with WNC Health Network and local health departments in western NC to vaccinate older adults, as well as the overall work of their organization and the community health worker model.
Learn more about UNETE at: https://unetenc.org/.
Erin: Will you please tell us a little about the work of UNETE?
Norma: Absolutely. UNETE is a very new organization. We started in 2021. So as new as it can be. The good thing is that we are rooted in two decades of grassroots effort and community work in our region – which was very, very helpful in securing a contract with NC DHHS Office of Rural Health. Because that investment in that grassroots work that allowed us to get the contract for a one year and renew for six months. And it was absolutely amazing, challenging, but amazing to be able to train and deploy 32 community field workers in our region in five counties.
Erin: And that contract was in response to the COVID pandemic.
Norma: Exactly, exactly. And it was such an experience and often I said we were building the plane while we were flying it. But, but – you know, the creativity, the commitment of people that want to become community health workers have to take the courses and pass the course and be certified was just inspiring. You know, you can relate with me – we didn’t think many many years ago that we would be executive directors – and here we are!
Erin: Norma, in addition to building and flying the plane during COVID, y’all were also partnering. So, can you talk a little bit about how during that time you were partnering with WNC Health Network?
Norma: We did, yes we did. And that was a great experience with the My Reason campaign. And we have one of our very fresh Community Care Workers sharing the experience, the reason why he got vaccinated… you know, every story you showed was inspiring. Of course when we go show one of our own, we love it. It was a great collaboration. We have it in so many meetings together, learning of the impact of using social media platforms, and supporting that work we do. Raising awareness. Prevention. Learning from you all and serving five counties. And we continue beyond that contract, which ended. We continue serving.
Erin: Well and speaking of continuing, we’re thrilled to be building on that partnership with the project that we’re doing now. So working more closely together on this project that we have funding from the National Council on Aging to support. So for the folks listening, this is a one year project that’s aimed at increasing COVID-19 and influenza vaccination rates among particularly our older, at-risk populations in our region.
We have three tracks of this project working together. So that raising awareness that you spoke about, understanding the importance of vaccinations through community-driven marketing, and education outreach. We’re also leveraging relationships with local health departments across five counties to increase access to vaccinations to clinics in some of their outreach. And then the part you’re here to talk about is connecting with individuals directly and building that trust within communities through that grassroots outreach that you all specialize in and have expertise in.
This project is really rooted in your community health worker model. I’d love for you to share with us what your experience has been so far working on this project. We’re about four months in. What have y’all achieved so far?
Norma: We are happy that we have achieved over 100 people vaccinated, which is wonderful. And you know, speak about how the community healthcare worker model is such an amazing tool. Even though we are so strategic in that our community health workers mirror the communities they serve, we were like woah the only one fitting the category of older adults on my team is me. So we were like “how is this going to work?” And I think the fact that they can identify with the sons and daughters trying to keep their parents or grandparents protected and healthy was a very important point of connection in outreach in this community. Also, you know, the skills and the talents and how seasoned our community health workers are.E verybody says “there is such an energy in their presence.” Basically because they believe what they are doing is real and tangible and is to keep people healthier and you know, living healthy lives to their full potential. And we know how certain illness, COVID-19 – the long effects that you will see, can affect all that. So, I think part of the success is, besides that we are you know in food distributions, we are present in free clinics, we have all these amazing relationships with health departments, and their support is so crucial in this matter. We are in agricultural places, in factories. Besides all that, what we are doing is that honest commitment and believing in our mission that we’re wellness for the whole person and the full community. Because…they just…a colleague said, “I love to be wherever UNETE is because the chances are that I leave with my belly filled, happy, and my soul too.”
Erin: That’s beautiful, Norma. That is really beautiful. And that you are sharing that embodied joy and commitment to supporting communities is just a beautiful thing.
So, I know that this work isn’t always easy. So what are some of the challenges that you’re facing with this project in particular?
Norma: The main challenge is related to the challenges of finding COVID-19 vaccines and vaccinators. Because we in our beautiful partnership with health departments we know they’re also facing their own challenges in providing these. And obviously before we have all these…we almost could choose, with the support of other organizations, you know vaccinators from here, vaccinators from there. Now there is not a pool to choose from. So, so that has been the greatest challenge right now. And also from free clinics and the health department, it is the same commitment to serve. So they bring us COVID-19 vaccines, they bring Shingles – very important for our elders to be protected. They also bring Tetanus and Hepatitis. So when the resources are there, the collaboration and the mutual support is very tangible. The problem is when they don’t have access to those resources. And obviously we provide non-clinician services so we have to rely on vaccines with the experts. So that has been a challenge that we wish we can do more to relieve the burden that some organizations are experiencing in this arena.
Erin: Norma, is there anything else you’d like to say about what you’re particularly feeling proud about with this work?
Norma: Mostly it’s the creativity of our community health workers team. The willingness of you all to share all these tools and platforms that we can use – the “View From Here”. Because we need everything we can put our hands on to, you know, keep doing these very challenging missions of serving through a lifespan – our community. Obviously UNETE is not doing this by ourself. I was sharing yesterday, in July only, we have reached over 1,200 people in our five counties. But, it’s not because we are doing it by ourselves, it’s because we are collaborating with so many organizations that allowed us to be present, offer our expertise, offer our resources, and outreach people and bring vaccines, bring information, and connect with resources. And the creativity, how our team, you know, “try this’ and “try that” and go to nursing homes or go to, I don’t know, places to get to know our elders and be there for them. So yeah, the understanding that this work is professional work but service too.
Erin: I really appreciate you lifting up just how wholeheartedly you and your team bring your expertise and your openness to engage and utilize the expertise of the health departments and the Health Communicators Collaborative. That is critical for us all to be able to serve our mission. So thanks for lifting that up.
Norma: We serve all, we serve all – we include pets in that “all.” We’ve vaccinated pets too! All means all.
Erin: Maybe even some elderly pets.
Norma: Absolutely. Of course, of course!
Erin: Before we go Norma, from what you and your team have learned across this project and through your years during the pandemic emergency, what advice do you have for communities trying to increase vaccinations?
Norma: Yeah, that is very very important. It’s just to tap into the wisdom of the community. The community knows what the community needs. The problem is who they are going to entrust with the knowledge to say, “This is what I need. And I want to let you know what I need. And I trust you. You are going to deliver those services, or connect me, with cultural humility.” It goes way beyond being from the same ethnicity or speaking the language. So just listen carefully and look for those representatives from that particular neighborhood, of that particular community that will be your allies and share wants, their needs, and the other one – the resources. Make that connection, build on that trust, and just be absolutely transparent. I will say what wrongly we call “communities difficult to reach,” we have very easy tools to outreach. Justas with any underserved sector of our population, we have these “tomb raiders” that we can tell when somebody is wholly present and committed or you know, there is some agenda. So I think, just be yourself, listen, and look for these crucial allies that they will trust you with their needs. And just remember to serve.
Erin: Well thanks so much for your time today, Norma. And thank you for trusting this partnership. We’re so grateful to be working with you to help build healthy and thriving people and communities in western North Carolina. For those of you listening, please stay tuned in our newsletter, we’ll be sure to give updates on how this project is finishing up. Thank you Norma.
Norma: Thank you, Erin. See you soon.
In January, 2023 Adrienne Ammerman (WNC Health Network) interviewed Meron Abebe (Operations Manager & Improvement Specialist, WNCHN) and Hannah Robinson Michael from Partners Aligned Toward Health about our organizations’ work together as it relates to Results-Based Accountability.
Learn more about PATH at: https://pathwnc.org/. Learn more about WNCHN’s RBA trainings here.
Meron and Hannah, let’s start with some introductions. Please each of you tell me a little bit about who you are – your role at your agency and the kinds of things you do day-to-day.
Meron: My name is Meron, Operations Manager & Improvement Specialist at WNC Health Network. The kinds of things I do, day to day include: Budget and financial management and reporting; Contracts; Policies and compliance, and General monitoring and accountability of organizational performance measures. I also provide support to our clients, like PATH, specifically around the implementation of evidence-based evaluation frameworks and qualitative data gathering and analysis.
Hannah: My name is Hannah and I’m the Healthy Lifestyles Program Manager at Partners Aligned Toward Health or PATH. PATH is a nonprofit. We use collaborative approaches to improve the health and wellbeing of families and community members in Mitchell and Yancey counties. Our initiatives shift as the community identifies new health needs but over the last several years, we’ve focused on healthy wellbeing and substance misuse prevention. In my role, I support a variety of programs, including the Healthy Yancey Coalition, Summer Food Program, and the Burnsville Fit Families 5K to name a few. I also support the data and evaluation work for PATH.
Meron, can you tell us at a high level what Results-based accountability is?
Meron: RBA is a way of thinking, organizing, and taking action in a disciplined manner. It is used to plan, evaluate, and improve projects, programs, and community-wide efforts. It helps people describe the contribution their work makes to the health and wellbeing of their community. RBA has been recognized as an evidence-based practice for evaluation and planning by the CDC, the National Institute of Health (IHI), and NC DHHS. In western NC, RBA is being used by hospitals, public health agencies, nonprofits, funders, and other local and regional partners in community health.
Hannah, how is PATH interested in Results-Based Accountability? What feels valuable about using RBA in your work?
Hannah: When people hear you support data and evaluation efforts for an organization some people’s eyes glaze over or they feel intimidated or there is general disinterest in the topic. We really had a desire to be able to talk about data and evaluation in a way that engages people and the RBA framework provides a commonsense approach that makes data and evaluation easy to understand regardless of your background. We also realized that internally, we needed a shared language around our work, our impact, and data & evaluation in general. The RBA framework has helped us do that and this makes moving our evaluation work forward much easier. Another major bonus of using the RBA framework is that funders have become interested in it. Sharing how PATH is using RBA has been beneficial on our grant applications and in general conversations with funders.
What made your team decide to reach out to WNC Health Network, and what kind of support were you looking for?
Hannah: Before I started at PATH, the organization was interested in improving their data and evaluation efforts to better demonstrate the impact that PATH is having on the community.
This led some staff to attend the regional RBA trainings hosted by the Network. This was helpful for building a general foundation in the framework and making an organizational switch to using RBA with all of our programs. Most recently, Meron and Emily led a PATH specific RBA training. This was great because it allowed all of our staff to be trained on RBA and they were able to use examples relevant to PATH throughout the training. We’ve also worked with the Network to develop evaluation plans for some of our specific programs. As the person on PATH’s staff that generally facilitates conversation around evaluation, it was extremely helpful to work with the Network because they laid out the plans for the meeting and facilitated conversation. I felt like I could more effectively participate in these conversations because I didn’t hold the dual role of facilitator and participant. The Network was there to hold the space. Being a part of developing these evaluation plans as a participant has build my confidence and my capacity to better lead these conversations with my team in the future. The last thing I’ll share is that WNCHN works with organizations throughout the region so they are able to share how our work and measures align with our partners through-out the region and the state. It’s been helpful for us to see how our work fits into the larger picture of the region.
Meron, Tell us a little bit more about what this partnership with PATH looked like from WNCHN’s end. [Do you have anything to add about] what kind of support you and our team provided on this project?
Meron: Our team has worked with PATH for many years on multiple projects. Last year, we provided evaluation support for two of their programs – Cougar Fit Club and Appalachian Youth to Youth. We reviewed existing strategy activities and measures and used the RBA framework to facilitate 5 evaluation workgroup meetings. We led the group through the first several steps of the RBA performance accountability decision making process to create an evaluation plan. And – during the process, we coached the team in developing and prioritizing performance measures and creating a data development agenda. We also provided a tailored virtual RBA training for PATH team members with a focus on RBA knowledge, use, and infusion into their specific projects and activities. We had 4, 2-hour sessions, spread over 4 weeks. We also administered a pre-and post-training organizational assessment tool, analyzed the data, and shared the findings with PATH.
How does this kind of project align with WNCHN’s values and approach for how we work in the region?
Meron: We bring our values to all our work with all clients. For instance, with the evaluation project and the RBA training, we co-designed the tools and materials we used with PATH and coached their team throughout, because we wanted to make sure that we are meeting their unique needs and building their capacity, rather than just BEING capacity, as that supports and sustains locally led improvements.
Wrapping up – Hannah, what’s next? How do you plan to use what you learned?
Hannah: Our next steps are to continue using RBA in our work and imbedding it into the overall functioning of the organization. We’re also eager to continue using our evaluation tools to get feedback from our customers so we can improve our work and ensure we’re meeting the needs of our community.
We also welcomed a new staff member at the beginning of the year so we’ll be sending Jacquie to an RBA training. She will be taking over our Home Remedies program. The program is an online course that introduces participants to strategies for pain management and stress reduction, all of which are presented by local complementary health providers. This program is paid for through an opioid response grant from the state so we’ll be working with Jacquie to update our evaluation tools using the RBA framework
Any words of wisdom or suggestions for other local organizations or agencies that want to infuse RBA into their work?
Hannah: PATH’s work with WNCHN focused on infusing RBA at the program level first. Later, we were able to train all of our staff in the RBA process. I’d recommend that organizations prioritize training staff on the RBA framework first, then honing in on specific programs. I’d also recommend training your entire staff if you can, not just your data people because the benefit of creating a shared language about evaluation is invaluable.
Meron: In 2023, we plan to hold two virtual RBA trainings, that we call “Getting to Results”. The first one is in February and the second one is in September. People who are interested can go to our website at www.wnchn.org and find RBA Training under the “What we do” tab. They will find a registration link on the bottom of that page.
Thank you both so much for sharing with us about this experience.
View the data slides here.
Eileen Tallman (WNCHN MPH Spring/ Summer ’22 Intern, Indiana University, Richard M. Fairbanks School of Public Health) and Jo Bradley (WNCHN Data Manager & Improvement Specialist) recently spoke with each other about their work together on a substance misuse data analysis project which involved analysis of single and polysubstance use emergency department (ED) visits in the 18-county region of WNC.
Adrienne Ammerman (WNC Health Network Communications & Improvement Specialist)
Hi, Jo. Hi, Eileen. So, we’re going to get started with our conversation today with just some introductions if you could both tell me who you are, what your role is and a little bit about what you do day to day…
Jo Bradley
I’m Jo Bradley. I’m the Data Manager and Improvement Specialist here at WNC Health Network. And one of my big jobs is collecting and curating the regional data for our 16- to 18-county region. And so that’s what’s going to lead us into Eileen here.
Eileen Tallman
I was a graduate intern with WNC Health Network before I graduated with my Masters of Public Health degree in August. Day-to-day I worked with data, looking at substance misuse in emergency departments in western North Carolina.
Adrienne Ammerman
Eileen, how did you first hear about the Health Network?
Eileen Tallman
I moved to the Asheville area recently and I was looking for ways to get involved in the community, and also meet the requirements for my Capstone project so that I could finish my program, and I found WNC Health Network. I felt it would be a great fit, especially because of the focus on health disparities. And I also really wanted to learn about regional initiatives… In school you talk a lot about national or state or community level health data, but not a lot about regional work. So I thought that was really interesting.
Adrienne Ammerman
Great. We’ve been happy to have you. Let’s talk a little bit about the research that you did.
Eileen Tallman
I knew that I wanted to do something that maybe I could contribute some they were useful information to the region. So in order to do that I needed to learn about racial health priorities. Which Jo can actually talk more about.
Jo Bradley
I’m going to go ahead and share my screen here… And what you should be seeing is a chart of our regional health priorities for the 2021-2023 CHA [Community Health Assessment] cycle. And you’ll notice that many of our counties identified substance misuse, mental health, followed by obesity, healthy eating, active living and nutrition. When we were deciding where we really wanted to start with this project, we went to the [health topic] that was selected by the most counties here in our region, which is substance misuse. So we started there, and then Eileen can tell you a little bit more about how we dug into exactly what we were going to study.
Eileen Tallman
We chose substance misuse, [which is] a very pressing issue. And based on some research that’s already been done, I learned that polysubstance use, or using two or more substances at the same time, is becoming more important, but we really haven’t had the data to study it very well. North Carolina Department of Health and Human Services recently added poly substance misuse as a priority of the state’s opioid and substance abuse action plan. And we had emergency department data. We knew that substance misuse was a driver of emergency department visits, we just didn’t know whether there were differences between people who were using a single substance going to the emergency department, or people who were using two or more substances. So for our analysis, we compared those. We also looked specifically at people who were using opioids, cocaine, or psychostimulants. So psychostimulants are things like methamphetamine. And those were, again, a local priority.
Adrienne Ammerman
And did you have any other partners for this research that you did?
Eileen Tallman
We worked with Dr. Jennifer Runkle, who works at North Carolina State University. She’s an environmental epidemiologist, and she served as a subject matter expert and helped us facilitate that data, provide some technical guidance.
Adrienne Ammerman
Great. So what were some of your high level findings?
Eileen Tallman
What we did find overall, was that substance misuse is increasing in the emergency department for residents of western North Carolina. Overall, we found that between 2016 and 2020 there was a 5% increase across those five years. And we also found, interestingly, that rural residents were coming into the emergency department visit more for poly substance misuse over time. So you can see on the graph that between 2016 and 2019 there was an increase of 5% of people coming in using two or more substances from rural areas. But if you look between 2019 and 2020, interestingly, there’s another 5% increase. We also saw that compared to emergency department visits for opioid and cocaine, psychostimulant-related emergency department visits were on the rise. That’s not a general finding about substance misuse in general in the community. That is the percentage when you compare to opioids and cocaine. And then, overall, we saw that percentages of opioid and psychostimulant emergency department visits nearly doubled for patients reporting as Black or African American who were residents in western North Carolina.
And lastly, we also looked at some other characteristics of the patients coming into the emergency department. So compared to individuals who came in for a single substance, western North Carolina residents coming into the emergency department for poly substance misuse were more than 26 times more likely to have a diagnosis of a mental illness and 76% more likely have been with suicidal ideation or behavior. And we did control for intentional overdoses in that data. They were also two times more likely to have housing or economic problems.
We found some specific differences in individuals coming in using cocaine or psychostimulants. So individuals using cocaine were six times as likely to have a mental illness. And patients coming in for psychostimulant use were more than four times as likely to have a mental illness. They’re also more likely to have housing or economic problems. And this was the group that was most likely to be living in a rural counties.
Basically, we wanted to share what providers can do with data like this, some of this data that’s available. So hospitals and emergency services can use the data to better understand who are coming in to their emergency departments. And we can get important demographic information about the types of individuals who are using specific substances when they come in. Researchers, epidemiologists, and analysts can use data to focus on regional analyses, which is so important. We have a lot of state and national level analyses, but they maybe don’t share insights that are specific to an area. They can also study polysubstance use. Again, this is a topic that more and more people are talking about. But it can help influence funding policy and programs. Substance misuse programs can also make use of data that can help them better understand who are coming into the EDS, so they can better prepare maybe when they make referrals. And informaticists – so those are folks who use data information and knowledge to improve human health and healthcare delivery – they can help make data more accessible so that these groups who may not have the expertise or may not have an easy way to get this data, they can help facilitate.
Adrienne Ammerman
Thank you so much for that high level overview of the research that you did, and how it can be used in our region and for people who are doing this kind of work. Jo, I’m curious how did this project align with the kinds of data projects that we do at the at the Health Network, and our values for how we work with data?
Jo Bradley
Clinical data has long been a data gap for our region, and being able to look at it at the regional level, all the facilities information at one time. And so when we found this opportunity to work with Eileen who’s really interested in hospital data and work with Jen Runkle has been amazing at being in this region, and had access to the data we saw it as a perfect way to kind of dip our toes into the water of clinical data and looking at regional data that way. And we know it’s something that people have been wanting for a long time and have been requesting, and we started with the most important health priority across our region. So that’s just one way that we’re trying to give back to the region.
Adrienne Ammerman
And Eileen, what was your experience like working with the Health Network on this on this research project?
Eileen Tallman
I had a very easy time when I got to work closely with Jo. It was just super responsive and gave me a lot of guidance. So it was a great experience. And, you know, it was a combination of working together and working independently. And I just learned a ton, especially about the region and community health.
Jo Bradley
I think about working with hospital data, there’s a lot of things that I learned as well about what needs to be in place to work with hospitals data and all the analysis.
Adrienne Ammerman
What’s next for you, Eileen?
Eileen Tallman
I’m continuing to dig in a little bit into this data because I was very time limited to get it done for my school project. But we’re continuing to work on that. And also, I’m looking for my next role in public health. So I’m very excited… I just got my degree, so I’m looking for opportunities in community health that will help me make use of my research background and my new skills.
Adrienne Ammerman
Awesome. We can’t wait to see what you end up doing and hope it’s in our region. Jo, I guess on a final note, how can people find out more about WNC Health Network’s data and Data Program?
Jo Bradley
The best place to start is our website [www.wnchn.org]. And we have a specific data section where you can download our full regional data set – that’s our primary and secondary data. That was just updated [in September 2022]. So you’ve got the latest, greatest data there. You can also sign up for our newsletters so that you keep getting information about data releases, we’ve got a lot of really good stuff that’s going to be released over the next year. And then of course, if you’re interested in getting involved or learning more, you can email me at jo.bradley@wnchn.org.
Adrienne Ammerman
Great, thank you so much for sharing about this project and great work.
By Nelle Gregory, RN, MPH
Many chronic health conditions and most dental diseases are preventable if we eat healthy foods, exercise, get good sleep, limit our stress, and practice good oral hygiene. Many of us have the information we need to make good decisions, so why do we sometimes

fail to follow our healthcare providers’ recommendations? To make changes in our behaviors, we must have the desire to act and move towards a goal…we must be motivated. For healthcare providers, it can be discouraging when patients fail to comply with their treatment recommendations. Research has shown that most of us have a hard time following our healthcare provider’s recommendations; knowledge is not enough to change behavior. It requires that healthcare providers move from simply sharing health information to building mutual respect that allows the patient to articulate his or her own solutions.
At community listening sessions conducted by The WNC Children’s Oral Health Initiative, parents said they do not know what good oral health looks like, when they should take their child to the dentist, where they could get care, what the standard care is, and how much it should cost. They do not have the basic information they need to make good oral health decisions… and it is impacting their ability to get their children into care. Many parents shared stories of feeling shamed and talked about being ‘blamed for their kids poor oral health.’ They discussed how this made them less likely to want to go back to the dentist.
The American Dental Association (Health Literacy in Dentistry, 2009) encourages the creation of a respectful and ‘shame-free’ dental environment. By helping patients identify their own reasons to change their behavior, they build trust in and respect for their healthcare provider and are more motivated to change. Motivational interviewing is one tool that helps healthcare providers support and encourage their patients’ readiness to change.
Motivational Interviewing (MI)
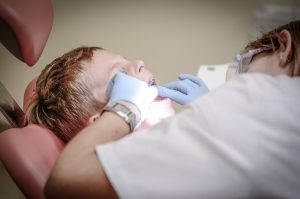 Motivational interviewing (MI) is an evidence-based approach to behavior change that is grounded in a respectful conversation between provider and patient to identify a patient’s readiness for change, and that helps the patient come up with ideas about how they can strengthen their motivation to change. Making MI the foundation of anticipatory guidance assures that providers listen to the concerns of parents and children, understand their ambivalence to change, and support their ideas about change and what they think would work. In a dental setting, MI shifts the conversation from a one-way monologue about brushing their teeth and cutting down on sugar to a conversation about the parent and child’s experiences, challenges, and ideas about what needs to change and how the provider can support them in making the needed changes.
Motivational interviewing (MI) is an evidence-based approach to behavior change that is grounded in a respectful conversation between provider and patient to identify a patient’s readiness for change, and that helps the patient come up with ideas about how they can strengthen their motivation to change. Making MI the foundation of anticipatory guidance assures that providers listen to the concerns of parents and children, understand their ambivalence to change, and support their ideas about change and what they think would work. In a dental setting, MI shifts the conversation from a one-way monologue about brushing their teeth and cutting down on sugar to a conversation about the parent and child’s experiences, challenges, and ideas about what needs to change and how the provider can support them in making the needed changes.
The American Dental Association research has shown that the main reason people do not get dental treatment is due to cost and perceived need. The way providers counsel impacts their patients’ perceived needs. At one of the community listening sessions a parent shared that her dentist told her to ‘just do a better job brushing her daughter’s teeth,’ but the parent, whose child is autistic, said that she has a hard time getting her daughter to open her mouth, and brushing her teeth is the least of her worries. She left frustrated that her dentist had no understanding of autism, and her perceived need for dental services was low.
Research has shown that using MI in dentistry can lead to more lasting behavior change and improved oral health outcomes (Kay, 2016). Positive behavior change occurs more readily when healthcare providers connect the change with what the patient values – people are motivated to change when it impacts what they value rather than what someone else determines they need. Confrontational styles or persuasion are likely to build resistance and mistrust. When health providers try to persuade or give advice, patients often feel guilt or shame. Healthcare providers must abandon the impulse to solve their patient’s problems and allow them to articulate their own solutions. Our motivation is impacted by our culture, family norms, and the multitude of other issues we deal with in our daily lives. The parent of the autistic child shared that she just needed her dentist to listen to her, hear the challenges she faces when trying to care for her daughter’s oral health, empathize with her, give her suggestions the dentist had heard from other autistic parents on how to get her daughter to open her mouth, and work with her to figure out a better solution.
Learn More
The WNC Children’s Oral Health Initiative is partnering with MAHEC to develop MI training for dental professionals. If you want to get more information about the project or MI training, contact nelle.gregory@gmail.com.
About the WNC Children’s Oral Health Initiative
The Western North Carolina (WNC) Children’s Oral Health Initiative, with funding from The Duke Endowment, is working to improve children’s oral health. The project is coordinated by Mission Children’s Hospital and WNC Health Network and overseen by a Steering Committee of dentists, dental hygienists, physicians, public health providers, and community partners. The group completed an assessment of children’s oral health in 18 western counties in NC in 2017. They held parent listening sessions to hear concerns parents in WNC had about their children’s oral health. A strategic plan was developed that prioritized the concerns voiced by parents.
References
American Dental Association. Health Literacy in Dentistry: Strategic Action Plan 2010-2015. Council on Access, Prevention, and Interprofessional Relations. Chicago, IL, 2009.
Achison KA, Rozier RG, Weintraub JA. Integrating Oral Health, Primary Care, and Health Literacy: Considerations for Health Professionals Practice, Education and Policy. Commissioned by the Roundtable on Health Literacy, Health, and Medicine Division, the National Academies of Sciences, Engineering, and Medicine. Prepublication copy, 2018.
Kay EJ, Vascott D, Hocking A, Nield H. Motivational interviewing in general dental practice: A review of the evidence. British Dental Journal 2016; 221: 785-791
Beth Booth, originally from the coast of NC, became health director of Graham County, NC in November, 2017. Since landing in her leadership role with Graham County Department of Public Health, she has led the agency in bringing back primary care and in streamlining services, working creatively to leverage auxiliary and support staff in the face of a rural nursing shortage.

Image by Nik Shuliahin
The health department is also strengthening their work in the community and has reestablished a previously dormant substance use coalition. In addition to Beth and Amber Williams, Health Educator at the health department, the coalition includes resource officers, principals, preachers, nonprofit leaders, the leader of Celebrate Recovery (a local faith-based recovery program), and the director of a local thrift store who is a minister and does work with substance use.
As Beth was getting the coalition back in action, she determined that she wanted to conduct a listening session (or focus group), with people in recovery to both help inform the community health assessment process, and to also avoid taking on issues not viewed as high priority by those most affected by substance abuse.
Beth and Amber worked with WNC Health Network before the listening session. “Support from WNC Health Network was crucial,” says Beth. “We attended their WNC Healthy Impact training on how to convene community listening sessions. Then they worked with us

Photo of Graham County by Patrick Williams, Ecocline Photography
one-on-one to develop the script and give us pointers, including how to pay attention to body language of people in the group, how to ask people to speak up without being obtrusive, and how to sit quietly and not overpower the group or sway them in any direction.”
Beth had built a relationship over the previous year with a team leader at Celebrate Recovery, and he was able to schedule an evening for Beth and Amber to come to meet with participants in the program. Beth and Amber arrived early so that they could participate in the sermon and group dinner prior to their session. “I didn’t just walk in during the middle of the sermon and disturb everything. Staying for the whole event is crucial for building mutual trust and respect,” says Beth.
Beth and Amber started their listening session by letting participants know that the session would be recorded, and how they were planning to use the information. When the session started they had six participants – by the time it ended they had about 10 in attendance.
“I told the participants – you are the experts in this. I want to know what you’ve experienced, how you got where you are, and how you got yourself out,” says Beth. “At one point when our tape recorder stopped running the participants let us know that it had stopped and waited to continue talking until the recorder was running again. Oftentimes public health is afraid they’re going to offend someone by asking targeted questions, but it’s not a sensitive issue to them, it’s their life. They want you to hear what’s coming out of their mouth and to give a darn about what they think.”
The listening session participants gave Beth and Amber feedback on where to locate syringe drop boxes, and how to best structure youth prevention programming. They also spoke to the challenges posed by stigma: “The group told me that there are plenty of people who have trouble getting help because people don’t think they’re worth the help.” Eventually, the team leader had to come in and stop the lively session because it was past 9 pm.
Because of feedback and insights gained from the listening session, the health department is now working on reopening the domestic violence shelter that shut down in 2017. They are exploring what can be done to expand transitional housing, and to increase prevention for youth, including resiliency education in the schools. They are looking at starting a support group for adults in recovery that is not faith-based, as well a support group for children located in the schools.
The experience – in addition to holding listening sessions with other segments of the community – has driven home for Beth that there are still too many people who don’t realize what a huge problem substance misuse poses for their friends, family, and neighbors. Beth says: “That has been an awakening for me – I took it for granted that people knew we have a problem in our county, but when I present the data and the stories I’ve heard you can hear the murmur going through the room… they’re shocked. It has started coming down to community-wide education and bringing everyone to realize, yes – there’s a problem in the county. It might not touch you, but it exists.”
Beth Booth’s Thoughts on Successful Listening Sessions:
If you are interested in learning how WNC Health Network could support you in conducting community listening sessions of your own, contact Emily Kujawa, Project Manager & Improvement Specialist (emily.kujawa@wnchn.org).

SIGN UP FOR OUR NEWSLETTER
