Percent of Adults Obese or Overweight in WNC, by Year
What do the numbers say about obesity?
Western North Carolina (WNC) Data:
In 2021, approximately one third (35.4%) of adults in WNC reported being obese (BMI of 30 or higher); of those adults 49% were diagnosed with high blood pressure, 33% were diagnosed with high cholesterol, 22% were diagnosed with diabetes and 25% reported fair/poor mental health in the past month.
The following adult populations were significantly more likely to be obese in 2021:
- Adults ages 40-64 years (40.1%)
- Low income (45.2%)
- Those identifying as Black (44.3%) or AI/AN, Indigenous (55.8%)
Only 23% of adults in WNC were meeting physical activity recommendations in 2021.
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Differences in health outcomes across social groups, economic status, and racial/ethnic identity are closely linked with disparities in social determinants of health, which disproportionately burden individuals and communities who experience systemic disadvantage and/or discrimination. See our data story on the social determinants of health to learn more about how the conditions in which people are born, live, work, play, learn, worship, and age can influence their ability to achieve good health for themselves and their families.
Percent of Adults in WNC Meeting the Physical Activity Guidelines, by Year
Meeting physical activity recommendations” includes adequate levels of both aerobic and strengthening activities: Aerobic activity is one of the following: at least 150 minutes per week of light to moderate activity, 75 minutes per week of vigorous activity, or an equivalent combination of both.
Strengthening activity is at least 2 sessions per week of exercise designed to strengthen muscles.
The percent of adults in WNC consuming 5+ fruits and vegetables per day has decreased from 8% in 2015 to 5.6% in 2021.
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Consuming 5+ Servings of Fruits & Veggies per Day, by Year
State and National Findings:
In 2017, North Carolinians had an obesity rate of 32.1%.
In 2015 and 2016, the prevalence of obesity in the US was 39.8% and affected about 93.3 million adults.
Obesity is a leading cause for many preventable chronic diseases that result in $147-$210 billion per year in healthcare costs in the US.
What did the region say is the story behind the obesity numbers?
Source: WNCHN – Online Key Informant Survey, 2018
The items below are paraphrased themes that emerged from a 2018 regional survey of key informants. These responses do not necessarily:
- Reflect accurate or scientifically validated information about health determinants, outcomes, and/or strategies for change.
- Represent an exhaustive list of factors that can help or hurt efforts to address this key regional health issue.
The information in this section should be interpreted and used with care. It should be used only to help local health departments and agencies begin to understand community perceptions about local health issues. Communities are strongly encouraged to collect their own, local-level data to inform local planning and evaluation activities.
What’s Helping?
- New greenways and parks
- Schools providing healthier food options
- Affordable and accessible recreation centers
- Walking trails
- Education in schools
- Bike lanes
- Increased awareness and education
- Increasing healthy produce access through food distribution sites and food pantry trucks
- Early education and intervention
- Offering healthy lifestyle classes
What’s Hurting?
- Lack of gyms or exercise programs for low income individuals
- Inability to access healthy food sue to financial resources
- Unhealthy cultural diets
- Challenges with healthy lifestyle changes
- Generational obesity
- Transportation barriers to exercise opportunities and healthy eating
- Cost of healthy foods
- Children growing up with too much screen time, poor eating habits and limited physical activity
- Food insecurity
- Lack of resources to maintain healthy lifestyles
What we are hearing:
“Educational programs around healthy lifestyles and food choices. Efforts for parks and access to fresh, local produce at a reduced cost. The effort to make parks tobacco-free. The fact that all students in our schools have PE classes every day.”
“[Evidence-based intervention programs] have demonstrated results in terms of addressing healthy eating. Nutrition is on the radar of many health advocates in the community and is being incorporated into the delivery of health care. Community gardens and other options for fresh produce are available.”
“We have become an “outdoor” community with a focus on biking, hiking, running/walking, etc. Outdoor education opportunities.”
“Sometimes people just cannot afford to buy the food they need to maintain a healthy lifestyle. The healthy foods are the most expensive.”
“Promotion of ‘quick fix’ programs that put emphasis on rapid loss of weight and a focus on overall weight as a number rather than a conscious move towards a more permanent healthy eating and physical activity lifestyle. A more holistic look at body composition and avoidance of disordered eating is needed.”
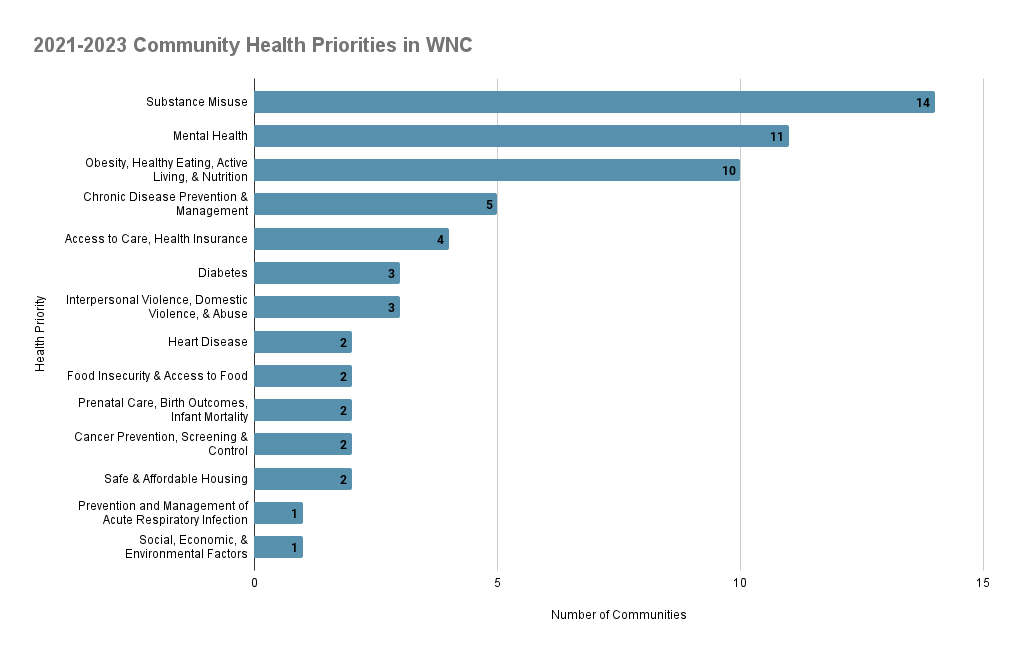
How is the region prioritizing this issue?
The western North Carolina region includes 17 communities: 16 counties and Eastern Band of Cherokee Indians (EBCI)
In the 2021 CHA cycle, 10 out of 17 communities chose a priority related to obesity, healthy eating, & active living. In addition, 5 communities prioritized chronic disease.
What is already happening regionally?
The list below represents a sample of what is happening in the region around this key health issue. Visit www.nc211.org for more resources.
- Safe Routes to School
- Double Up Food Bucks (MountainWise)
- Programming through the YWCA of Asheville, YMCAs of WNC, local Parks and Recreation departments, and Senior Centers
- Walk with Ease (various agencies, including Area Agencies on Aging and senior centers)
- Worksite Wellness grant (MountainWise)