Percent of Adults in WNC Dissatisfied with Life, by Year
Survey Question: In general, how satisfied are you with your life? (Very Satisfied; Satisfied; Dissatisfied; or Very Dissatisfied) “Dissatisfied” includes those who answered either dissatisfied and very dissatisfied.
What do the numbers say about mental health?
Western North Carolina (WNC) Data:
Approximately 10% of adults in WNC are dissatisfied with life. The following adult populations were significantly more likely to be dissatisfied with life in 2021:
- Very low income (23.6%) or low income (14.9%)
- Those identifying as Black (14.7%) or AI/AN, Indigenous (14.4%)
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Differences in health outcomes across social groups, economic status, and racial/ethnic identity are closely linked with disparities in social determinants of health, which disproportionately burden individuals and communities who experience systemic disadvantage and/or discrimination. See our data story on the social determinants of health to learn more about how the conditions in which people are born, live, work, play, learn, worship, and age can influence their ability to achieve good health for themselves and their families.
The percent of adults in WNC reporting that they “always or usually” get the social and emotional support they need has declined from 79% in 2015 to 70% in 2021.
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Always-Usually Get Support Needed, by Year
The percent of adults in WNC reporting that they did not get the mental health care or counseling that they needed in the past year has risen from 9.1% in 2015 to 10.6% in 2021.
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Unable to Get Needed Medical Care, by Year
The percent of adults in WNC reporting greater than 7 days of poor mental health in the past month has risen from 13% in 2015 to 22% in 2021.
(WNCHN – WNC Healthy Impact Community Health Survey, 2021)
Percent with More than 7 Days of Poor Mental Health in the Last Month, by Year
State and National Findings:
In 2013-2014, a survey of North Carolinians found that almost 5% of adults had a serious mental illness within one year of being surveyed. This was an increase from the previous survey that took place 2010-2011.
The estimated number of adults in the U.S. with serious suicidal thoughts is over 9.8 million—an increase of 200,000 people since the last data set.
Serious mental illness costs America an estimated $193.2 billion in lost earning per year.
What did the region say is the story behind the mental health numbers?
Source: WNCHN – Online Key Informant Survey, 2018
The items below are paraphrased themes that emerged from a 2018 regional survey of key informants. These responses do not necessarily:
- Reflect accurate or scientifically validated information about health determinants, outcomes, and/or strategies for change.
- Represent an exhaustive list of factors that can help or hurt efforts to address this key regional health issue.
The information in this section should be interpreted and used with care. It should be used only to help local health departments and agencies begin to understand community perceptions about local health issues. Communities are strongly encouraged to collect their own, local-level data to inform local planning and evaluation activities.
What’s Helping?
- Increased awareness in mental health issues
- Decreased stigma surrounding mental health issues
- Opioid Leadership Forums
- Increased availability to therapy and mental health counseling services
- Educating patients, families and the community
- Collaboration among behavioral health agencies, jails, social services, hospital, law enforcement, community members and families
- Extended hours for behavioral health providers
- Crisis lines and sliding fee scale mental health services
What’s Hurting?
- Limited resources in some areas
- Length of time it takes to schedule appointments at some agencies
- Needs exceed services available
- Fee-based services that individuals and families may not be able to afford
- Not enough 24/7 beds for deeply mentally ill
- Transportation challenges
- Limited addiction treatment across the state
- Lack of integrated behavioral health and primary health care programs
- Lack of mental health providers and high turnover
- Lack of funding for mental health services
- Stigma regarding mental health
What we are hearing:
“Our community has spent many hours collaborating and developing a strategic plan regarding behavioral health concerns. Agencies and community leaders are invested in making change occur and in helping our community become healthier.”
[A regional, comprehensive behavioral health care services agency], [a national grassroots, mental health organization], excellent youth programs in schools, camps, and county/private/nonprofit programs foster resiliency.”
“There are no resources available, and more and more people are experiencing mental health concerns because of media and technology.”
“Too many people go to jail or are involuntarily committed, which shows there are not services or current providers aren’t doing their job.”
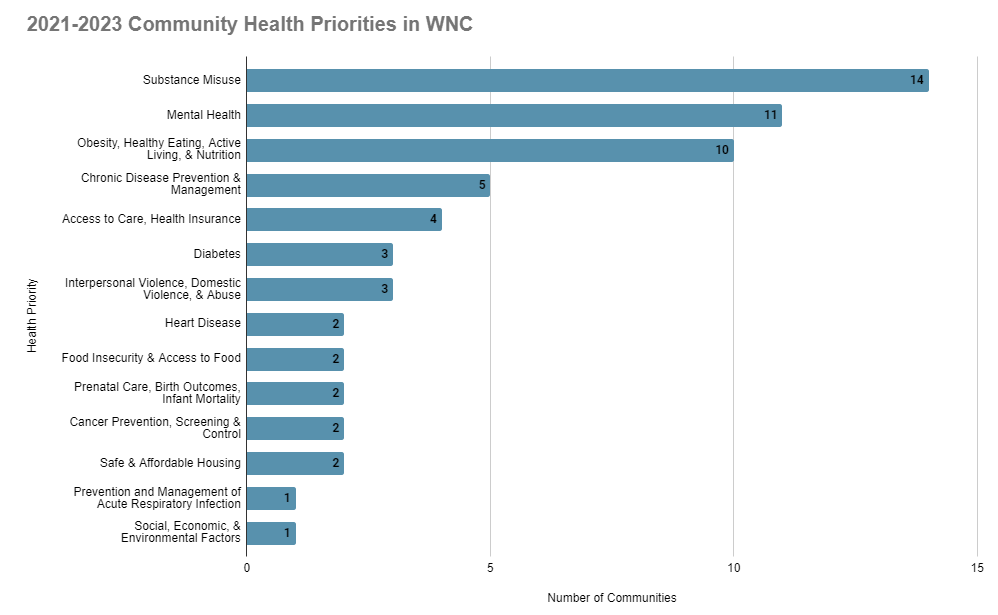
How is the region prioritizing this issue?
The western North Carolina region includes 17 communities: 16 counties and Eastern Band of Cherokee Indians (EBCI)
In the 2021 CHA cycle, 11 communities chose a priority related to mental health.
What is already happening regionally?
The list below represents a sample of what is happening in the region around this key health issue. Visit www.nc211.org for more resources.
- Crisis phone line and behavioral health urgent care (physically located in Asheville) (Vaya Health, in partnership with RHA, Mission Hospital, and others)
- Comprehensive Centers in the region (Family Preservation Services, RHA Health Services, Appalachian Community Services, Meridian Health Services, Blue Ridge Community Health). Note: these centers and providers may offer a range of services such as walk-in services, crisis teams/units, behavioral health urgent care, and recovery education.
- Inpatient units in hospitals (Mission Hospital, Haywood Regional, Pardee, AdventHealth, St. Luke’s, Rutherford Regional)
Broughton Hospital (state-operated psychiatric hospital located nearest our region, in Burke County). - FQHCs in the region provide mental health and substance use services (may do MAT): WNCCHS – ABCCM; Appalachian Mountain Community Health; Blue Ridge Community Health Services; Hot Springs Health Program; Bakersville Community Medical Clinic; Vecinos, Inc.
- Initiatives through National Alliance on Mental Illness of WNC
- Living Healthy with Chronic Pain Self-Management Program (CPSMP) (multiple agencies, including Area Agencies on Aging and NC Center for Health and Wellness)
- Resilience training and skills development resources (available throughout the state)
- DD Plus (Developmental Disabilities and Behavioral Health Integration in Primary Care Practices) (Pilot project sponsored by ARC, in partnership with Mission Children’s Developmental Peds, Hendersonville Peds, MAHEC Family Practice and McDowell Peds).
- Family Support Network (Mission Health)
- Developmental Pediatric Specialty Program (Mission Health)
- Adult Behavioral Health in Primary Care (Mission Health)
- Psychiatry residency program with training for rural practice (MAHEC)
- Behavioral health provider and school nurse education (in person and live video conference) (MAHEC)
The regional dataset (WNC Healthy Impact Community Health Survey and Online Key Informant Survey) is available thanks to contributions from hospitals in the 16-county region of western North Carolina. Thank you!